The VHHA Board of Directors approved making publicly available a Virginia report card that measures aggregate quality and patient safety performance of Virginia's hospitals. Information contained herein details progress made by Virginia hospitals and health systems in select quality and patient satisfaction elements of performance. The improvement targets are reflected in the Virginia scorecard.For CLABSI, Virginia aims for a 50 percent reduction from current infection rates. For CAUTI, readmission, mortality and patient satisfaction, the target is for Virginia to be among the top five states in each measure. We recognize that this target will move over time as every hospital and state pursues improvement as well.
Having accurate data is essential for the pharmacy director to manage the department and develop patient-centered pharmacy services. A balanced scorecard (BSC) of essential department data, which is a broad view of a department’s function beyond its financial performance, is an important part of any department’s strategic plan. This column describes how the pharmacy director builds and promotes a department’s BSC. Specifically, this article reviews how the BSC supports the department’s mission and vision, describes the metrics of the BSC and how they are collected, and recommends how the pharmacy director can effectively use the scorecard results in promoting the pharmacy. If designed properly and updated consistently, a BSC can present a broad view of the pharmacy’s performance, serve as a guide for strategic decision making, and improve on the quality of its services.
Hospitals and health systems are required to measure and track performance due to government, private, and consumer pressures to ensure quality health care services. Hospital value-based purchasing (HVBP) programs, meaningful use incentives, and the Patient Protection and Affordable Care Act (ACA) are examples of programs that force accountability and quality of care while reducing overall health care expenditure. Pharmacy directors face significant challenges with rising drug costs and limited pharmacy staff while being expected to provide the highest quality pharmacy services. To meet these expectations, the pharmacy director must balance resources and performance. They must show how they have achieved that balance. Essential department data can be effectively used to help measure the success of the department in meeting their strategic goals, which are ideally aligned with the organization’s priorities.Balanced scorecards (BSCs) are used in health care to list the results of the delivery of health care services as a continuous quality improvement approach.
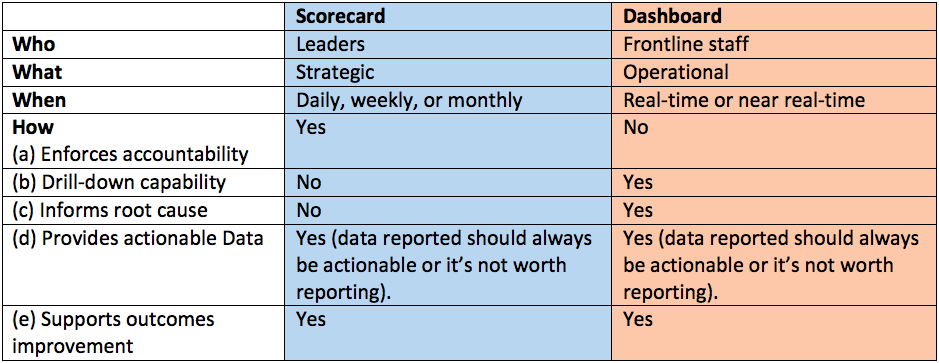
The BSC was first introduced in 1992 by Kaplan and Norton as a way to view performance broadly rather than a narrow focus on financial measures., The BSC contains 4 perspectives: customer, internal process, innovation and learning, and financial. The BSC was first discussed as a tool to be used in health-system pharmacy as a way to demonstrate pharmacy’s value in meeting its key performance metrics. In addition, BSCs were introduced in 1999 to improve medication use and to manage resources devoted to drug therapy. The BSC is often divided into sections that reflect the key operations of a pharmacy department, including medication safety, operations, quality, finance, education, and research.The terms BSCs and dashboards are often used interchangeably, but these tools are distinctly different. BSCs trend performance metrics over longer time intervals of weeks, months, and quarters; dashboards, track performance over shorter intervals in minutes, hours, and days. Dashboards typically serve as tactical indicators on the state of a process and focus on action limits involving trend lines instead of progress toward prespecified goals.
A BSC is often structured to measure organizational performance metrics based on specific strategic goals, which offer better information for making decisions for the pharmacy department.,This article highlights the key metrics that pharmacy directors should include in the design of their pharmacy department’s BSC. The goal of this article is to provide hospital pharmacy directors with a method to develop a successful BSC that can be used to promote patient-centered pharmacy services. This article describes the importance of using a BSC to support the department’s mission and vision; lists and reviews the specific metrics used within the BSC to monitor medication safety, operational efficiency, quality improvement, education, research initiatives, and financial performance; and describes ways the pharmacy director can promote pharmacy services using the BSC. This article also reinforces the BSC concepts by describing The Ohio State University Wexner Medical Center’s (OSUWMC) success in developing and implementing a BSC. BSC and the Department’s Strategic PlanEffective strategic planning is essential for a health-system pharmacy to meet its goals. The pharmacy director must collaborate with stakeholders to reach a common understanding regarding the goals, priorities, initiatives, and future direction for the pharmacy department.
To what extent has the Balanced Scorecard been introduced in healthcare? Health examples of Balanced Scorecard implementation found elsewhere. A healthcare KPI or metric is a well-defined performance measurement that is used to monitor, analyze and optimize all relevant healthcare processes to increase patient satisfaction. Many of these metrics are actually specific key performance indicators for hospitals. Here is the complete list of the most important healthcare KPIs and metrics, that we will discuss in this article in every detail.
Traditionally, the pharmacy director promoted this understanding through personal discussion, newsletters and memos, presentation with stakeholders, and staff meetings. The BSC contains a measure of various programs and processes that reflect the strategic plan of the pharmacy department. The BSC is another way for the pharmacy director to correlate the results of the department to its mission, vision, and plan. Portrays the relationship of the BSC in supporting the department’s strategic plan. The pharmacy director must be able to effectively articulate the purpose of implementing a BSC for the pharmacy department and how it can serve as an up-to-date benchmark for strategic goals.
Elements of the BSCDeveloping a pharmacy department BSC is an intricate process, and the pharmacy director must understand the difference between a dashboard and a BSC when considering what metrics to use for external and internal benchmarking., A dashboard focuses on graphical monitoring of operational processes; a BSC includes detailed measures that closely align with organizational strategic goals and objectives. Based on the considerations discussed earlier in the article, it is recommended that the pharmacy director incorporate Kaplan’s four broad perspectives in creating the department’s BSC.Performance measures are differentiated as leading and lagging indicators. For example, the number of peer-reviewed articles submitted for publication represents a leading indicator, which is a driver of the lagging indicator, the number of peer-reviewed articles accepted for publication. Lagging indicators are commonly associated with financial metrics that represent historical performance based on actions taken.
The scorecard will most likely be a combination of both leading and lagging indicators.The pharmacy’s leadership team, in cooperation with the other stakeholders (eg, nursing, physicians, C-suite), should brainstorm to determine what performance measures the BSC should evaluate so that it provides relevant, valid, and trusted data. Once the metrics have been identified, individuals should be assigned to collect and analyze data for the BSC. Baseline data should be obtained to assist with establishing performance target goals for each measure. Local and national benchmarks should be used, as these are often validated; in addition they add a sense of credibility to the BSC results.
The frequency for updating the BSC should be determined at the outset (ie, monthly, quarterly, and yearly). Then results can be compared to the previous time-frame and noted on the scorecard to visualize progress.Most commonly, BSC metrics are focused in the areas of medication safety and quality, pharmacy operations, research, education, scholarship, and financial performance. At OSUWMC, the following elements of the BSC were established: medication safety and quality, pharmacy operations, education and research, and finance. Medication Safety and QualityAn area of opportunity for health-system pharmacy departments is the elimination of medication errors. The pharmacy director can identify key performance metrics that can be tracked on a BSC, such as total reported medication errors and number of pharmacy-attributed harm and nonharm errors.
Medication errors are stratified by the process nodes (storage, ordering, preparation/dispense, administration, and monitoring). Improvement in medication safety, for example, is shown by a downward trend in harmful medication errors while maintaining a consistent reporting of overall errors.At OSUWMC, the pharmacy department’s primary medication safety goal is to reduce harmful medication errors. As a result, the medication safety BSC metrics were to reduce number of pharmacy attributable medication errors by 10% of fiscal year 2013 baseline; implement all of the 2014-2015 Institute for Safe Medication Practice (ISMP) best practices for medications in hospitals; and expand the “grass-root” medication event review team program to at least 75% to 85% of hospital areas.Other pharmacy services that reflect and impact the quality of care should be highlighted on the BSC. For example, important clinical functions such as medication order interventions, dosage adjustments, medication reconciliation activities, and specific drug therapy monitoring should be tracked. There are at least 5 medication-specific core objectives out of 16 indicators in Meaningful Use Stage 2; the pharmacy department can track their progress on these objectives through a BSC.
Pharmacy OperationsPharmacy directors utilize internal and external benchmarking systems to carefully optimize pharmacy operations, and these systems should be incorporated into the BSC. The University HealthSystems Consortium (UHC) serves as a valuable resource to allow pharmacy directors to compare their department to other similar peer institutions. Action OI (Thomson Reuters Corporation, New York) is an external benchmarking reporting organization that is available through UHC; it is designed to provide participants with comparative operational and financial data of hospital departments with similar demographics. Examples of the benchmark data include hours worked/unit of service, skill mix, labor and supply expense/unit of service, and other operational practices. The use of key Action OI measures on the BSC provides a quick view of the performance of the department’s operations compared to peers. Pharmacy directors are often requested to establish internal benchmarking metrics; internal productivity monitoring systems avoid inappropriate comparison with dissimilar organizations and allow pharmacy departments to accurately assess workload volume related to staff activities and practice changes.Other important operation indicators that a pharmacy director should report through a BSC include STAT and routine verification time, automated dispensing cabinet (ADC) percent capture rate, ADC stock outages, and total inpatient doses dispensed and returned.
After establishing goals for each of these internal metrics, the pharmacy department’s performance can be tracked on a monthly, quarterly, and yearly basis to ensure compliance. In addition, electronic health information systems provide opportunities for enhanced data capture, thus allowing problematic issues to be investigated all the way down to specific end-users.The OSUWMC BSC tracks fundamental operational measures. This was facilitated through the implementation of the hospitals’ integrated health information system (IHIS, which is an Epic platform) in 2011. One of the pharmacy department’s strategic goals is to continually refine IHIS to meet and exceed the medication needs of the patients. As a result of IHIS, OSUWMC was able to more reliably capture pharmacist verification times and establish targeted goal verification times of 15 minutes and 60 minutes for STAT and routine medications, respectively. These data are automatically collected from IHIS and are then exported from a database into the BSC each month. Education, Research, and ScholarshipThe integration of students and residents into a pharmacy department’s practice model is essential in order to empower pharmacists to practice at the top of their license; this is strongly supported in ASHP’s Practice Model Initiative.
The BSC measures fundamental elements such as the number of pharmacy department peer-reviewed publications and Introductory and Advanced Pharmacy Practices Experience (IPPE, APPE) student rotations.At the OSUWMC, the pharmacy department achieves its strategic goal of scholarship by empowering the pharmacists to contribute to the overall body of pharmacy knowledge. Pharmacists are encouraged to provide Accreditation Council for Pharmacy Education (ACPE)-level continuing education to the department of pharmacy on a monthly basis.
In addition, the OSUWMC pharmacy department has established initiatives to increase the number of peer-review submissions, book chapters, and accepted resident manuscripts by a specified percentage each year. Financial PerformanceDrug and personnel costs are the 2 main expenses that a pharmacy director must track closely. Drug costs are rapidly increasing each year, and they make up the majority of pharmacy department expenses. According to the ASHP Foundation 2014-2018 Pharmacy Forecast report, drug shortages, specialty pharmacy medications, biosimilars, and pharmacogenomics will have a huge impact on drug costs going forward. In addition to monitoring purchasing trends, the pharmacy director should monitor drug costs in relation to patient days, admission, discharge, volume, doses dispensed per admission, and pharmacy costs as a percentage of total hospital costs.,In regard to personnel costs, a BSC can be used to track hours worked per unit of service, labor cost per admission, labor expense per doses billed, pharmacist worked hours per order, technician worked hours per dose, clinical interventions per pharmacist shift worked, and pharmacist to technician skill mix ratio on a monthly, quarterly, and yearly basis. This type of monitoring and analysis will help the pharmacy department flex staff appropriately and optimize care for the patients.Ultimately, the OSUWMC strives to achieve its financial goal by serving as a benchmark pharmacy practice model.
OSUWMC 2014 financial initiatives center on achieving the pharmacy department’s cost-reduction goal, implementing a specialty pharmacy service, and reorganizing the practice model to help meet the needs of the Medical Center Expansion Project. At OSUWMC, the following financial metrics were incorporated into the BSC: total cost of medications dispensed per case mix adjusted day, cumulative cost reduction, and overtime expense. Case mix adjusted day was designed to take into account the high acuity of patients and their need for more medications at an increased frequency. Moreover, the pharmacy director should be able to use both internal and external metrics to track the progress toward achieving the department’s strategic goals.shows an example of a BSC. The BSC can be placed into a Microsoft Excel or Word format, with links to various databases to facilitate the ease of updating. Key directivesPerformance measureGoalJune 2014Fiscal YTDCommentsMedication safetyTotal medication events reportedDaily, monthly, quarterly, and yearly reported medication events by type, cause, severity, and drug class↑ReportingNo. Promoting Pharmacy Services with the BscAdvocacy is an extremely important role for the pharmacy director; this advocacy is external (to legislators, payers, public health groups) and internal (C-suite, nursing, physicians).
The pharmacy director can use the BSC as a talking point to demonstrate the impact of the pharmacy service on overall hospital goals.The BSC allows the pharmacy director to share the department’s success with hospital leaders and educate staff about metrics that trend performance over time. Because the strategic plan is updated on a yearly basis, the BSC metrics should be evaluated annually to determine whether the current process should be continued, modified, or discarded or additional metrics added. In addition, the pharmacy director can highlight the pharmacy department’s BSC performance metrics that are associated with patient-centered pharmacy services to other hospital administrators each month, thus keeping them abreast of the department’s progress. This sharing of the pharmacy department’s BSC will help all members of the pharmacy department continually gauge strategic goal achievement and objectively demonstrate the value of clinical pharmacy services.
ConclusionA well-designed pharmacy department BSC is an effective tool that can consistently track the progress of the pharmacy department in achieving the hospital and department’s strategic goals. It is important for the pharmacy department to design BSC metrics that are meaningful, credible, and validated.
These metrics must also be easily monitored to track progression toward the department’s strategic goals. A BSC can be used to justify clinical pharmacy services and promote the pharmacy department, if the pharmacy director can clearly communicate its correlation with the institution’s mission, vision, and strategic goals.
If designed properly and updated consistently, a BSC presents a broad view of the pharmacy’s performance, serves as a guide for strategic decision making, and improves the quality of its services.
 RSS Feed
RSS Feed
