An insulin pump is a small, pager-sized device that delivers a continuous dose of insulin through a cannula to cover your baseline or background insulin needs. When you eat food that contains carbohydrate you will have to deliver a bolus of insulin via the pump based on the amount of carbohydrates you've eaten. It is important that you understand how to physically operate the device so that you deliver the right amount of insulin. You will have to understand carbohydrate counting, too, because insulin doses for meals are dependent on how much carbohydrates you've eaten. You will receive something called an insulin-to-carbohydrate ratio. The insulin to carbohydrate ratio will determine a specific amount of insulin based on the carbohydrates in your meal.
Like many questions, to “pump or not to pump” has multiple correct answers. In reality, some people are surprised to find out that the insulin pump gives. Professional to determine whether you're a good candidate for insulin pump therapy.
For example, if your insulin to carbohydrate ratio is 1:10 that means you need one unit of insulin for every 10 grams of carbohydrates eaten. Therefore, if you eat 40g of carbohydrate you will bolus 4 units of insulin. Again, insulin pumps are not meant for all patients with Type 2 diabetes. Newly diagnosed patients, patients with well-controlled diabetes on oral medications or those patients with are not good candidates for pump therapy. Also, those patients on very large doses of insulin should not be prescribed an insulin pump.
If you are someone who needs to take more than 25 units of insulin for your meals, then a pump is not for you. Insulin pump reservoirs are filled with fast acting insulin, but depending on the pump the reservoir can hold on average anywhe.
Continuous subcutaneous insulin, or the insulin pump, has gained popularity and sophistication as a near-physiologic programmable method of insulin delivery that is flexible and lifestyle-friendly. The introduction of continuous monitoring with glucose sensors provides unprecedented access to, and prediction of, a patient’s blood glucose levels. Efforts are underway to integrate the two technologies, from “sensor-augmented” and “sensor-driven” pumps to a fully-automated and independent sensing-and-delivery system. Implantable pumps and an early-phase “bionic pancreas” are also in active development. Fine-tuned “pancreas replacement” promises to be one of the many avenues that offers hope for individuals suffering from diabetes. Although endocrinologists and diabetes specialists will continue to maintain expertise in this field, it behooves the primary care physician to have a working knowledge of insulin pumps and sensors to ensure optimal clinical care and decision-making for their patients. IntroductionDiabetes is rapidly becoming a major health epidemic in most regions of the world.
All patients with type 1 diabetes and a significant number with type 2 diabetes require the use of insulin for controlling blood glucose. In the last 20 years, technological innovation and bioengineering has transformed the diabetes therapeutic landscape. There are several varieties of insulin and many different injection regimens that can be used.
However, in spite of the availability of insulin vials and pens, the acceptability for patients and the glucose readings that are obtained with the use of single or multiple-dose injection regimens is not to the desired level. Insulin delivery with pumps, also known as continuous subcutaneous insulin infusion (CSII), was introduced almost a half century ago. It utilizes short- or rapid-acting insulin types only, thus minimizing variability of administration and reducing the chances of glucose fluctuations. Pump technology has progressed to the level of precisely mimicking physiological demands. Programmable insulin administration in basal and bolus fashion is integrated and augmented with glucose biosensors to provide real-time, data-driven glycemic control and early detection of hypoglycemia.
The prospect of a functional, closed-loop “artificial pancreas” with implantable or bionic capabilities is now within the realm of technological possibility in the near future. How Do Insulin Pumps Work?Insulin pumps deliver insulin by continuous infusion through a single subcutaneous site which is replaced, on average, every three days. Only rapid-acting insulin is used, and the analogue insulins have gained popularity over regular insulin for this purpose. A pump delivers programmable basal insulin around the clock which is tailored to the patient’s 24-h glucose profile. The insulin requirements may be affected by the individual’s physiology, the type and duration of daily activity, work schedule, exercise, illness, concomitant medications, etc. Most patients utilize multiple basal rates over a 24-h period, but some may use a single rate. Almost all pumps have the capability of programming basal rates that are modifiable every hour and also have a temporary basal rate feature for special situations.
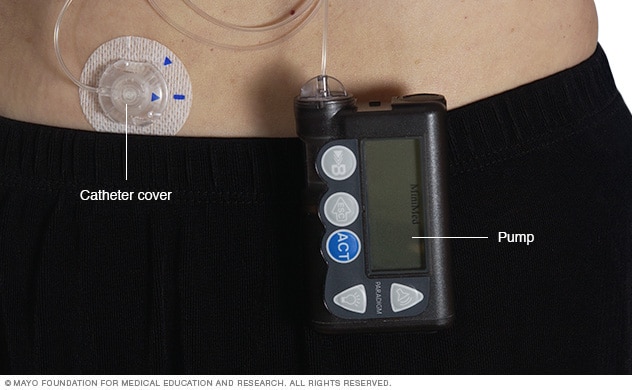

Patients can also deliver bolus insulin which infuses over a few minutes to a few hours. Insulin boluses cover meals and correct for high blood glucose levels. For the pump to accurately calculate bolus insulin amounts, the carbohydrate content of food and the blood glucose level are required. Insulin delivery via the pump can be suspended by the patient if necessary.
Evolution of Insulin Pump TechnologyThe first insulin pumps were bulky machines that were employed only for research purposes. Pumps were commercialized for use in the general diabetic patient population in the 1970s. They required patients to calculate the amount of bolus insulin for food coverage and for high glucose readings.
Technological capabilities have advanced dramatically since that time, and pump use has increased manifold. Statistics show that an estimated 350,000 people in the United States (US) use insulin pumps today, and about 30,000 of those are believed to have Type 2 diabetes. Currently available pumps deliver basal insulin in increments of as little as 0.01 units per hour, and use automatic bolus insulin calculators. Although the pump and its supplies (insulin cartridges, tubing, and infusion sets) remain expensive, insurance coverage has improved considerably over the years. With phenomenal advances in self-monitoring of blood glucose, meters are able to communicate the readings directly and wirelessly to the pump via infrared technology, thus eliminating the extra step of manual entry of the glucose value into the pump by the patient. The Medtronic Minimed and the Animas Vibe brands are examples of some of the more commonly prescribed insulin pumps ( and ). Touch screen technology and user-friendliness have been incorporated in Tandem diabetes Care’s T-Slim insulin pump.
Tubeless and fully disposable pumps provide a desirable option for many patients (OmniPod Insulin Pump, ). On average, an insulin pump costs about US $6000 and supplies between US $3000 and $6000 annually. Patients who switch from multiple-dose insulin injections (MDII) to pumps in a managed care setting realize a reduction in insulin expenditures of around US $657 per year. Potential Benefits of Pump TherapyThe expected benefits of insulin pump therapy are summarized in. Insulin pump use provides a near-physiologic basal-bolus insulin delivery method that, in theory, mimics normal pancreatic function better than injections.
Precise insulin dosages can be programmed and administered, giving the patient increased flexibility in daily living with regard to mealtimes, travel, work schedule, etc. Observational studies, meta-analyses, and randomized clinical trials have demonstrated improvements in long-term glycemic control when compared with daily multiple-dose insulin injections ,. Evidence from clinical studies suggests that pump therapy is associated with a decreased risk of severe hypoglycemia and the need for emergent medical care. The latter translates into reduction in the cost of care and utilization of health care resources.
 RSS Feed
RSS Feed
